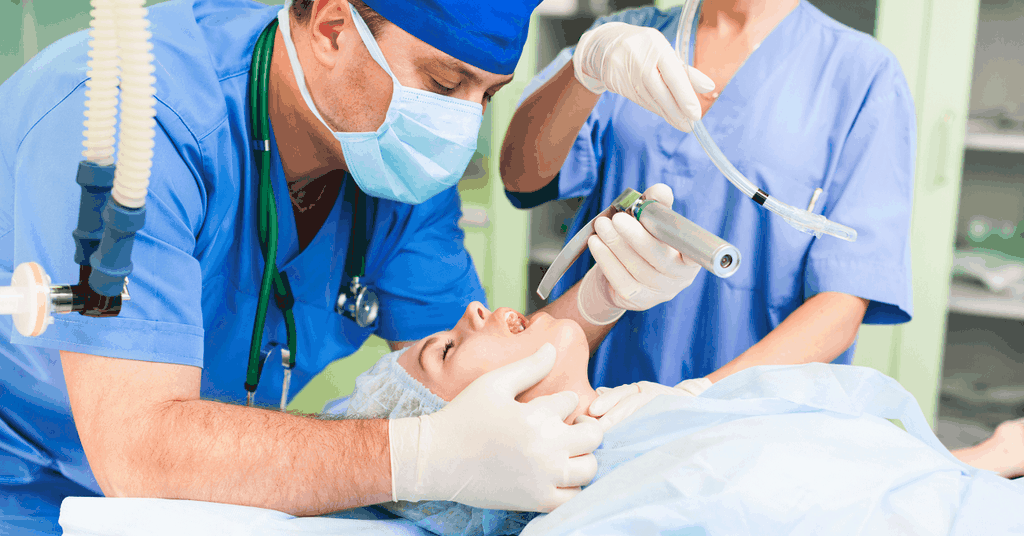
Acute Care Nurse
Click for background info

Click for background info
This is the daily diary of an acute-care nurse at a London hospital treating Coronavirus patients on a daily basis. We hope to be bringing you daily updates as and when possible. Please undersatand there may be gaps in the diaries.
It is an unfiltered, honest and accurate account of what is really happening on the ground - How many cases are there? Can our NHS cope? How bad is this, really?
Nurses, doctors and many other medical staff are fighting, every single day, on the frontline of the COVID-19 crisis.
Leave comments with messages of support
Life on the wards.
Day 42
As expected more people are out and the majority are heading back to work. Of concern for those of us in London who use TFL, the trains have not being deep cleaned and haven’t been since the start of this pandemic. However in New York they have been shutting down the subways for a deep clean quite often throughout! So anyhow what can we do to protect ourselves and more importantly to protect others?
Yes wearing a mask is a sensible idea while using public transport, if a mask is not available a cloth which you are happy to dispose of could be used instead. Once you are off the train/bus TAKE THE MASK OFFF without touching the main front part, then get rid of it! Make sure you wash your hands afterwards.
Wearing gloves is another common question/thought. I have seen people doing this, however if you are wearing a glove that touches a contaminated surface then you go to grab your phone to text your friend??? Think, you are protecting your hand but then continuously spreading whatever you have touched!
It is very simply wash your hands often, do not touch what you don't not need to! Just think and go slowly that's the best advice I can give.
Think when you are out and about:
What am I doing?
Do I need to be outside first of all?
Am I going into a confined area?
Am I protecting my mouth from air droplets?
If you do have to touch a rail or bar, wash your hand as soon as you can, wipe down your phone with a surface wipe.
As a disclaimer this is my advice to protect yourself, the government has provided Grey matter information (no surprise there). It is a lot of common sense this information which you are all capable of doing. Just simply think and plan ahead.
Stay safe!
Day 40
Yes wearing a mask is a sensible idea while using public transport, if a mask is not available a cloth which you are happy to dispose of could be used instead. Once you are off the train/bus TAKE THE MASK OFFF without touching the main front part, then get rid of it! Make sure you wash your hands afterwards.
Wearing gloves is another common question/thought. I have seen people doing this, however if you are wearing a glove that touches a contaminated surface then you go to grab your phone to text your friend??? Think, you are protecting your hand but then continuously spreading whatever you have touched!
It is very simply wash your hands often, do not touch what you don't not need to! Just think and go slowly that's the best advice I can give.
Think when you are out and about:
What am I doing?
Do I need to be outside first of all?
Am I going into a confined area?
Am I protecting my mouth from air droplets?
If you do have to touch a rail or bar, wash your hand as soon as you can, wipe down your phone with a surface wipe.
As a disclaimer this is my advice to protect yourself, the government has provided Grey matter information (no surprise there). It is a lot of common sense this information which you are all capable of doing. Just simply think and plan ahead.
Stay safe!
Day 40
It has all changed here at my hospital, normality is slowly returning to my ward but I fear a different version. From the continuous demand from patients walking through A & E we now see just a few stroll through. We actually had the lowest amount of patients recorded on Wednesday!
Tonight on TV is a show called ‘air a documentary’ which I strongly recommend. I myself was a part of this program and it just puts into perspective the situation in very visual terms. I think the timing is perfect. Before you use this 'unlimited exercise' excuse please watch this documentary and question whether for yourself you agree with the new terms of the current lockdown.
Deaths are still averaging out to 300-400 daily depending on the day of the week.
This documentary was filmed from the start of the Coronavirus outbreak and throughout the peak. Yes we have moved on from that situation now. However there is still a need for social distancing in order that we do not to return to that dreadful situation. I understand the economy needs a human input in order for an economic output to be maintained. However we have the second highest death rate in the world, look at our population of 66 million people -on an island!
Tonight on TV is a show called ‘air a documentary’ which I strongly recommend. I myself was a part of this program and it just puts into perspective the situation in very visual terms. I think the timing is perfect. Before you use this 'unlimited exercise' excuse please watch this documentary and question whether for yourself you agree with the new terms of the current lockdown.
Deaths are still averaging out to 300-400 daily depending on the day of the week.
This documentary was filmed from the start of the Coronavirus outbreak and throughout the peak. Yes we have moved on from that situation now. However there is still a need for social distancing in order that we do not to return to that dreadful situation. I understand the economy needs a human input in order for an economic output to be maintained. However we have the second highest death rate in the world, look at our population of 66 million people -on an island!
Day 31
So I've had the last few days off, simply being, enjoying the weather and trying out some new recipes. My ward itself has now become a 'clean ward' which is a good sign I guess as they are managing COVID patients.
It's all a bit weird because the admissions to A&E have definitely declined. However due to the nature of this disease, ITU is still at full capacity. ITU being full does have an effect on the other patients who do not have COVID 19 but still requiring ITU care.
It was a strange feeling not to be in Full PPE when caring for an individual. However wearing surgical face masks is a requirement before going within a 2 meter area of any patient to protect them from us as well.
To hear a certain shop will trial opening again, I am concerned that it will cause a second peak. However the general public still need to adhere to social distancing and to do necessary shopping only! However I do believe the rules will be bent as people see more and more shops opening.
Personally I wouldn't want any non-essential shops to open until ITU beds are starting to empty and become a bit more relaxed. I wonder why they don’t limit it to drive through only fast food restaurants rather than the fast food stores.
While walking along the high road yesterday it was comforting to see the majority of stores still closed. I do understand there is an economic rationale behind all of these decisions however lives are still at risk, surely that overrules economics?
Day 27
It's all a bit weird because the admissions to A&E have definitely declined. However due to the nature of this disease, ITU is still at full capacity. ITU being full does have an effect on the other patients who do not have COVID 19 but still requiring ITU care.
It was a strange feeling not to be in Full PPE when caring for an individual. However wearing surgical face masks is a requirement before going within a 2 meter area of any patient to protect them from us as well.
To hear a certain shop will trial opening again, I am concerned that it will cause a second peak. However the general public still need to adhere to social distancing and to do necessary shopping only! However I do believe the rules will be bent as people see more and more shops opening.
Personally I wouldn't want any non-essential shops to open until ITU beds are starting to empty and become a bit more relaxed. I wonder why they don’t limit it to drive through only fast food restaurants rather than the fast food stores.
While walking along the high road yesterday it was comforting to see the majority of stores still closed. I do understand there is an economic rationale behind all of these decisions however lives are still at risk, surely that overrules economics?
Day 27
Last night as I finished my shift at 8pm I found myself walking into a ‘clap for careers’ outside the hospital main doors. It was quite over whelming and re-energised me at the end of a long shift. Thank you to all of those out there that are taking the time to do this. Yesterday was especially memorable as on top of the ‘clapping’ ice creams were donated and delivered to the staff canteen. The ice creams were a welcome distraction which uplifted everyone's mood.
So this morning I am heading off to start another day shift, the energy and vibe of day shifts is so different to working nights. Today I will be caring for a mixture of patients in lots of different specialties, these sorts of shifts are both challenging and rewarding as they help me to develop new skills.
At my hospital now the majority of wards have become mini intensive care units, I think many hospitals have adopted the same approach to deal with the level of care that COVID19 patients require. It has been breath-taking to see the way the whole hospital has adapted and changed to meet the challenge and I feel proud to be a part of it.
So this morning I am heading off to start another day shift, the energy and vibe of day shifts is so different to working nights. Today I will be caring for a mixture of patients in lots of different specialties, these sorts of shifts are both challenging and rewarding as they help me to develop new skills.
At my hospital now the majority of wards have become mini intensive care units, I think many hospitals have adopted the same approach to deal with the level of care that COVID19 patients require. It has been breath-taking to see the way the whole hospital has adapted and changed to meet the challenge and I feel proud to be a part of it.
Day 25
Tonight was my final night on my current shift cycle, there are definitely noticeably less admissions from A&E. However ITU is still at full capacity with patients.
In the hospital we are all slightly worried that people with normal conditions such as chest pain are not presenting to A&E where are they? Things that we can deal with as early interventions in A&E are not being treated. We are worried of the long term impact this will have people’s health.
Please understand that we have a system in place in the hospital to keep people presenting with COVID separate to non-COVID admissions. Staff testing is definitely improving more accessible, so that is a relief for us all to know we have proper access to testing if/when needed.
I'm looking forward to a few days off recharging my batteries so I can get back in the saddle. But for the next few days the plan is to sit in the sun, do a bit of painting and to catch up with my family.
In the hospital we are all slightly worried that people with normal conditions such as chest pain are not presenting to A&E where are they? Things that we can deal with as early interventions in A&E are not being treated. We are worried of the long term impact this will have people’s health.
Please understand that we have a system in place in the hospital to keep people presenting with COVID separate to non-COVID admissions. Staff testing is definitely improving more accessible, so that is a relief for us all to know we have proper access to testing if/when needed.
I'm looking forward to a few days off recharging my batteries so I can get back in the saddle. But for the next few days the plan is to sit in the sun, do a bit of painting and to catch up with my family.
Day 22
Just spent the last couple of days relaxing, in the garden chilling out, family barbecue, I even did a bit of painting. I just needed some time without having to say the “C” word if you know what I mean.
As a nurse part of my job is managing the way the patient feels about their situation. Each patient is different, so it’s important knowing how to give the right information for each patient.
I am often asked:
- What is my prognosis?
- Please can you tell me what to expect?
- How serious is it?
But I have to tell them that no 2 patients have exactly the same symptoms or even pre-existing conditions. At the same time I try to reassure them that they are in the best possible place.
But then again there are other patients that just don’t want to know anything, they just want to be treated without being given the details.
Then there is the other group of patients who come in, usually in a lot of distress it’s sad to see the severe panics attacks. In most cases their fear of having COVID19 has driven them into a mental health crisis. They genuinely think they have it and are terrified. By the time they get to us the ambulance paramedics have already spent time trying to reassure and calm them.
But event though they are having a panic attack they might still be asymptomatic with COVID19. So we treat these patients in exactly the same way. Starting with looking for any danger signs, but we have to be more sympathetic, building up trust, checking for COVID19 symptoms. Only then can we determine if it is a mental health or medical emergency.
I am looking forward to going back to the ward again, I just needed a little break. The management team putting our shifts together are doing a great job, allowing us enough time for R+R so we are all ready to go again.
I have gone past panic now over COVID19, I know that I can’t control things out side of me. But I can control my mind set, I can take responsibility for how I feel.
I am actively present in the moment and I know that I am doing something positive about what is going on in the community. The thing that has been most important for me is facing it head on. I have learned to deal with it and through that knowledge I have become better at helping my patients.
Day 21
I have just finished 3 days of back to back shifts on the ward, phew! The management of COVID-19 is becoming clearer as each day passes. We have formed more of a process now, which has definitely developed my confidence, in caring for a patient with COVID-19.
It will be the fourth “Clap for our careers” at 8pm tonight! Get ya pots and pans out and make a good old racket!! I for one really appreciate hearing this. Thankfully a well needed 2 day break is approaching, the weatherman says that the sun is staying with us so that will be great.
Unfortunately, now a new 'crisis' within the pandemic is coming about because the UK still lacks enough PPE and we also have a lot of outdated kit, it's truly upsetting. That said, I must admit I am very fortunate not to have experienced this situation vat my hospital. To any other nurse out there who is lacking proper PPE, I honestly hope & pray this is not a situation that continues for much longer!
The new 3 week Government lockdown came as a relief to myself and colleagues, I can’t tell you how anxious we were at the thought of a 'relaxed lockdown' moving forward. Thankfully companies such as the big supermarkets are now conscientiously attempting to ensure the 2 metre social distance rule is finally being observed in the aisles. We all have to do our bit in keeping our communities safe.
Finally - the sun is out, so even if you don't have a safe outside area to sit in, please do make sure you try to sit by an open window and feel the sun on your skin.
Unfortunately, now a new 'crisis' within the pandemic is coming about because the UK still lacks enough PPE and we also have a lot of outdated kit, it's truly upsetting. That said, I must admit I am very fortunate not to have experienced this situation vat my hospital. To any other nurse out there who is lacking proper PPE, I honestly hope & pray this is not a situation that continues for much longer!
The new 3 week Government lockdown came as a relief to myself and colleagues, I can’t tell you how anxious we were at the thought of a 'relaxed lockdown' moving forward. Thankfully companies such as the big supermarkets are now conscientiously attempting to ensure the 2 metre social distance rule is finally being observed in the aisles. We all have to do our bit in keeping our communities safe.
Finally - the sun is out, so even if you don't have a safe outside area to sit in, please do make sure you try to sit by an open window and feel the sun on your skin.
Day 19
I have found my last few shifts have been tough, and relentless due to the constant stream of new admissions with COVID-19. It is very noticeable just how disproportionately the coronavirus affects more men than women.
We are now receiving a constant supply of yummy cookies and other treats which just make it that little bit easier to cope. Also realising that there have now been 3 events of 'clap for the NHS' is actually quite a shock as it really does not feel like 3 weeks since this lockdown began.
I had been seeing far less people on the roads which was reassuring, unfortunately over the Bank Holiday weekend there were a lot of people who just didn't follow the Government regulations. This is so disappointing for me to see!
I am very happy to say that my hospital has been great with PPE and I haven't had any issues in accessing PPE to protect myself. For my colleagues in other essential services who are struggling, I am truly upset that you are not being protected and I hope this changes as soon as possible.
Day 15
This is a morning entry for today, as I am back on day shift.
I am back at work this morning, it is great to be back on the frontline and playing my part. I do somewhat feel guilty when I'm not at work these days. To counter this I try to occupy myself with other hobbies & house jobs. Over the last few days if have been keeping myself distracted in a positive way by decorating my room.
The ward is just managing a few of our specialty patients, but it is mainly covid-19 now. It is great to see the discharge list for the day, the patients that are able to go home and see their families! This gives a real sense of hope for all of us.
I work with such an amazing team who I can't thank enough for keeping up my spirits and all of the support that they give to me.
Day 14
I’ve just worked three night shifts in a row and to be honest last night was a bit heavy…
A lot of patients passed away, which meant we were doing a lot of palliative care on our ward. But the issue is that because this virus is so new, we were trying to learn the best way to do it on the job, which obviously isn’t ideal. The shit has well and truly hit the fan. We’re getting towards the peak of this now.
We were getting continuous admissions from A&E and the majority were end of life care. We see a lot of patients getting delirious because of a lack of oxygen going to the brain, and we are giving them as much oxygen as possible but people are so confused that they often unconsciously take their oxygen mask off.
Another issue is that when a patient requires urgent CPR, we have to get fully kitted up in protective equipment before we can treat them. So this means we have to leave someone with no pulse or sign of life while we get our kit on, which reduces their chance of survival.
Having done three night shifts in a row I’m actually really looking forward to working the day shift tomorrow, there’s more people around to give you a hand.
Another issue is that when a patient requires urgent CPR, we have to get fully kitted up in protective equipment before we can treat them. So this means we have to leave someone with no pulse or sign of life while we get our kit on, which reduces their chance of survival.
Having done three night shifts in a row I’m actually really looking forward to working the day shift tomorrow, there’s more people around to give you a hand.
Day 13
There has been a lot of uproar and media coverage about a lack of protective equipment for NHS staff, but I don’t really see that. At my hospital we have to get changed in the toilets because the changing room is full of PPE, but that’s just my hospital and I can’t say for sure if it’s the same everywhere else.
We have regular briefings from an Infectious Diseases Doctor on our ward and they’re telling us that the reason so few medical staff in Wuhan died from Coronavirus was because they seriously limited their use of PPE.
The fact is that if you’re fully covered in PPE throughout your shift, you don’t take it all off and replace it all the time. You might take your mask off, or leave it draped around your neck, or your gloves…but you keep some of it on.
That means you’re breaking the chain of infection and it can spread more easily. So the theory is that if you only wear PPE when you directly need it, then you remove it entirely, it could actually reduce the spread.
All staff are offered psychological support as well, if they want it, and at 4am someone played Bob Marley through our walkie-talkies, which was brilliant! And someone even delivered warm cookies…No matter how bad the day is, there’s always something good to take out of it!
We have regular briefings from an Infectious Diseases Doctor on our ward and they’re telling us that the reason so few medical staff in Wuhan died from Coronavirus was because they seriously limited their use of PPE.
The fact is that if you’re fully covered in PPE throughout your shift, you don’t take it all off and replace it all the time. You might take your mask off, or leave it draped around your neck, or your gloves…but you keep some of it on.
That means you’re breaking the chain of infection and it can spread more easily. So the theory is that if you only wear PPE when you directly need it, then you remove it entirely, it could actually reduce the spread.
All staff are offered psychological support as well, if they want it, and at 4am someone played Bob Marley through our walkie-talkies, which was brilliant! And someone even delivered warm cookies…No matter how bad the day is, there’s always something good to take out of it!
Day12
I worked a 12 hour night shift last night - it was mad, but it was controlled madness, if you know what I mean?
We’re learning more about this virus every day - we’re trying to identify trends but at the moment it feels a bit like a lottery.
We had a young, fit, healthy guy come in. He’s a builder, looks like he works out - doesn’t drink or smoke. At 8pm he was walking around, chatting and being normal. His signs were all good and he wanted to self-discharge. But then at midnight I literally had to pick him up off the floor and he needed urgent critical management. We were looking around like: ‘What did we miss?’ But I honestly don’t think we did miss anything. It seems like some people with Covid-19 will fluctuate massively and very quickly - so they’ll be fine one minute, and falling off a cliff the next, then when we gave this patient fluids and high flow oxygen he recovered again pretty quickly.
I understand the basic science behind Covid-19; what it does to the lungs, etc…but there are so, so many unknown around this. It’s like throwing pins at a board.
Every hospital has a Research Analyst who looks at the notes from every Covid patient so they can identify trends and we can learn more about this. Apparently there are 11 trends at the moment and it’s impossible to get to the bottom of any of them.
I must say that whenever there’s an emergency there is an influx of staff like I’ve never seen before. When someone gets really ill there’s a core team of people who go to them immediately: An infectious diseases doctor, a resuscitation team, an ICU doctor.
There’s been a lot said in the media about the lack of testing for NHS staff. My view is that anyone, not just NHS staff but literally anyone in the country, should only be tested if they have symptoms or have been exposed to a confirmed positive person. People have to understand that there is still a budget in an epidemic and what does it achieve if all NHS staff are tested every day? Firstly, it’s not feasible, but also think about this; If you test me today, in three days you will have the results. Well what about what happens in those three days? Do you test me again? It doesn’t make sense. We do have to be smart about how we use our resources.
I’m not sure whether or not this is the case in other hospitals or wards, but judging from last night it seems there are more men being affected by this than women. It also seems that renal patients are hit very hard. So, people who are on dialysis but are out in the community, there appears to be a disproportionate number of them suffering with Covid.
I must say that whenever there’s an emergency there is an influx of staff like I’ve never seen before. When someone gets really ill there’s a core team of people who go to them immediately: An infectious diseases doctor, a resuscitation team, an ICU doctor.
There’s been a lot said in the media about the lack of testing for NHS staff. My view is that anyone, not just NHS staff but literally anyone in the country, should only be tested if they have symptoms or have been exposed to a confirmed positive person. People have to understand that there is still a budget in an epidemic and what does it achieve if all NHS staff are tested every day? Firstly, it’s not feasible, but also think about this; If you test me today, in three days you will have the results. Well what about what happens in those three days? Do you test me again? It doesn’t make sense. We do have to be smart about how we use our resources.
I’m not sure whether or not this is the case in other hospitals or wards, but judging from last night it seems there are more men being affected by this than women. It also seems that renal patients are hit very hard. So, people who are on dialysis but are out in the community, there appears to be a disproportionate number of them suffering with Covid.
The morale among the staff is quite varied - there is definitely a togetherness and a sense of feeling quite strong. We all have walkie-talkies now so we can get in touch immediately with whoever we need to. It’s much more efficient and, to be honest, I think after all this dies down we should still use them!
Day 11
Tomorrow night I’m back at work, it's the start of three consecutive night shifts. To be honest, I’ve felt guilty and found it quite hard to accept that I’ve been at home for a few days while all this is going on but I appreciate that we’re all human and need a bit of time out.
The hospital knew that they could call me at any time if they needed me so in a way it’s good that they’re not just calling all staff in for no reason - they’re clearly managing relatively well at the moment.
My manager called and asked if I had any symptoms, which I don’t, so I’ll definitely be back in tomorrow!
I just want to make it clear that I don’t want to tell anyone what to do, but you shouldn’t present yourself at A&E unless you have to. A lot of the weird and wonderful things you see in the A&E department have slowed down, it’s mostly people displaying Covid symptoms.
If you go into A&E and you have Covid symptoms, in my hospital they are putting you in a Red Zone, so you are segregated from other patients - they’re clearly managing this relatively well at the moment.
Also, what’s happening now is that medical staff take their uniform off at the end of each shift and it’s put in a big bin. It’s then taken away by the cleaners and you get new scrubs at the start of each shift to try to cut back on the spread of Covid.
When I go back I’m on nights, and I’m expecting it to be busy. Often a lot of people feel ill during the day but say to themselves: “I’ll see how I feel in a few hours.” Then night time comes and they arrive, and they can be put on the wards so we can get anyone in any condition at any time.
I’m going to spend my final night off just eating loads and getting myself mentally ready. Bring on tomorrow night.
The hospital knew that they could call me at any time if they needed me so in a way it’s good that they’re not just calling all staff in for no reason - they’re clearly managing relatively well at the moment.
My manager called and asked if I had any symptoms, which I don’t, so I’ll definitely be back in tomorrow!
I just want to make it clear that I don’t want to tell anyone what to do, but you shouldn’t present yourself at A&E unless you have to. A lot of the weird and wonderful things you see in the A&E department have slowed down, it’s mostly people displaying Covid symptoms.
If you go into A&E and you have Covid symptoms, in my hospital they are putting you in a Red Zone, so you are segregated from other patients - they’re clearly managing this relatively well at the moment.
Also, what’s happening now is that medical staff take their uniform off at the end of each shift and it’s put in a big bin. It’s then taken away by the cleaners and you get new scrubs at the start of each shift to try to cut back on the spread of Covid.
When I go back I’m on nights, and I’m expecting it to be busy. Often a lot of people feel ill during the day but say to themselves: “I’ll see how I feel in a few hours.” Then night time comes and they arrive, and they can be put on the wards so we can get anyone in any condition at any time.
I’m going to spend my final night off just eating loads and getting myself mentally ready. Bring on tomorrow night.
Day 9:
I got a call from work to say that I won’t be going back in until Wednesday now because they need to make sure they keep a variety of different specialist staff on each ward. I’m still very up for going back, I enjoy my job and I want to be there. When I get back I’ll be doing 12hour night shifts.
I know a lot of nurses have been sent for advanced life support training and we now have proper PPE (personal protective equipment). It puts patients and yourself in a much safer environment and I know a lot of medical staff are more confident interacting with patients so that improves their quality of care.
There are still definitely not enough ventilators to cope going forward but it looks like they are coming and it appears the new 4,000 bed Nightingale Hospital in London is nearly ready so that is very reassuring. I think we may yet be able to avoid the projected 20,000 death toll, but we’ll have to see.
There will be a wait for the new ventilators and breathing equipment but obviously we need to make sure it’s properly tested before we can use it.
Apparently around 25,000 former NHS staff are going to return to work. They’ll definitely be needed because a lot of nurses don’t feel equipped to go to this new hospital, so it will rely heavily on experienced, returning medical staff. It’s expected that a lot of the returning NHS staff will go to the new hospitals to help there and many existing staff can stay where they are and help there.
At my hospital we are constantly trying to find new space for intensive care units. The high dependency unit has become a mini-ICU, as have many of the theatres and the recovery rooms.
I’m expecting there to be a steep rise in the death toll in the next couple of days and I don’t see it coming down any time soon but, like I said, we may be able to keep below the 20,000 figure that has been projected.
I know a lot of nurses have been sent for advanced life support training and we now have proper PPE (personal protective equipment). It puts patients and yourself in a much safer environment and I know a lot of medical staff are more confident interacting with patients so that improves their quality of care.
There are still definitely not enough ventilators to cope going forward but it looks like they are coming and it appears the new 4,000 bed Nightingale Hospital in London is nearly ready so that is very reassuring. I think we may yet be able to avoid the projected 20,000 death toll, but we’ll have to see.
There will be a wait for the new ventilators and breathing equipment but obviously we need to make sure it’s properly tested before we can use it.
Apparently around 25,000 former NHS staff are going to return to work. They’ll definitely be needed because a lot of nurses don’t feel equipped to go to this new hospital, so it will rely heavily on experienced, returning medical staff. It’s expected that a lot of the returning NHS staff will go to the new hospitals to help there and many existing staff can stay where they are and help there.
At my hospital we are constantly trying to find new space for intensive care units. The high dependency unit has become a mini-ICU, as have many of the theatres and the recovery rooms.
I’m expecting there to be a steep rise in the death toll in the next couple of days and I don’t see it coming down any time soon but, like I said, we may be able to keep below the 20,000 figure that has been projected.
Day 8:
Last night, millions of people went to their doorstep and showed their love for the NHS. Everyone on my road came out and I could hear cars beeping from miles away as well. It’s nice to know there’s a lot of appreciation out there and it's great to see everyone come together - whilst remaining a safe distance, obviously!
I'm keeping a positive outlook - I can't get ill, I can't get weak because that means one less nurse going to work every day. There isn't one individual nurse or medical professional who is going to solve all this on their own, but we're all sharing the load. So we're all taking a little bit of stress home with us. That way it doesn't all fall onto one person's shoulders and we can manage this.
I must say I'm not surprised to hear that Boris Johnson and Prince Charles have tested positive for Coronavirus because this illness doesn't discriminate based on any title, privilege, race, ethnicity, etc...
I'm back at work in a couple of days and I know that on my ward we've already had two nurses who have taken indefinite leave because they don't feel like they can hack the pressure. To be fair, they were relatively new to the profession and working on a liver transplant ward is stressful enough as it is, so they hadn't planned to deal with this as well.
My trust has set up a 24/7 helpline for staff. What's great is that no matter when you call that number, the person on the other end of the line is someone with direct experience of working in the NHS. So you don't have to explain things to them, they get it. Some people are struggling to sleep because of all this, and the phoneline helps massively for our mental health. We're also eating for free in the canteen at work every day now. I'm actually quite surprised by how generous people are.
I'm quite excited and ready to go back to work. Watching your colleagues dealing with this while you're on annual leave for a couple of days is really tough.
Even though people might not realise it, every nurse has a life outside of nursing! So I've been running, I'm redecorating my room because I wanted to give myself a mini project to take my mind off things.
We're expecting the 'peak' of this crisis to hit home in the next week or so, so there is still a long road ahead with so many unknowns.
I'm keeping a positive outlook - I can't get ill, I can't get weak because that means one less nurse going to work every day. There isn't one individual nurse or medical professional who is going to solve all this on their own, but we're all sharing the load. So we're all taking a little bit of stress home with us. That way it doesn't all fall onto one person's shoulders and we can manage this.
I must say I'm not surprised to hear that Boris Johnson and Prince Charles have tested positive for Coronavirus because this illness doesn't discriminate based on any title, privilege, race, ethnicity, etc...
I'm back at work in a couple of days and I know that on my ward we've already had two nurses who have taken indefinite leave because they don't feel like they can hack the pressure. To be fair, they were relatively new to the profession and working on a liver transplant ward is stressful enough as it is, so they hadn't planned to deal with this as well.
My trust has set up a 24/7 helpline for staff. What's great is that no matter when you call that number, the person on the other end of the line is someone with direct experience of working in the NHS. So you don't have to explain things to them, they get it. Some people are struggling to sleep because of all this, and the phoneline helps massively for our mental health. We're also eating for free in the canteen at work every day now. I'm actually quite surprised by how generous people are.
I'm quite excited and ready to go back to work. Watching your colleagues dealing with this while you're on annual leave for a couple of days is really tough.
Even though people might not realise it, every nurse has a life outside of nursing! So I've been running, I'm redecorating my room because I wanted to give myself a mini project to take my mind off things.
We're expecting the 'peak' of this crisis to hit home in the next week or so, so there is still a long road ahead with so many unknowns.
Day 7:
So I'm on annual leave until Sunday evening when it's back to work. I've just tried to switch off from it all as best I can. All the medics on my ward try to stick to a rule of not speaking about it too much! I do now have confidence that there will be much faster Coronavirus testing soon. Do I feel time has been lost? Yes, absolutely. But this is the thing: Until you've actually seen the reality of Covid-19 on a day to day basis, like medical staff do, then it will probably take you some time to appreciate how serious this is.
A new hospital is being built at the ExCel Centre in London, it will have the capacity to treat 4,000 intensive care patients. Even if it doesn't end up being used by that many patients, just knowing it's there and that we're planning, preparing and investing in ways to fight this virus...it's really reassuring.
Obviously, everyday, Boris briefs the nation on what's happening. Professor Chris Whitty, our Chief Medial Officer, is usually with him. To be honest, what's coming out of his mouth seems like total sense. But, that said, I still think he should speak to more nurses who are just coming off a night shift. See how they feel. What are they saying about this situation? I don't think they want to admit that there IS a lack of equipment, there IS a lack of staff, facilities, space...they don't want to admit that.
Don't get me wrong, I completely understand that those in power have to try to keep everybody calm at the moment, but I'd like the 'experts' to meet with more frontline staff.
A new hospital is being built at the ExCel Centre in London, it will have the capacity to treat 4,000 intensive care patients. Even if it doesn't end up being used by that many patients, just knowing it's there and that we're planning, preparing and investing in ways to fight this virus...it's really reassuring.
Obviously, everyday, Boris briefs the nation on what's happening. Professor Chris Whitty, our Chief Medial Officer, is usually with him. To be honest, what's coming out of his mouth seems like total sense. But, that said, I still think he should speak to more nurses who are just coming off a night shift. See how they feel. What are they saying about this situation? I don't think they want to admit that there IS a lack of equipment, there IS a lack of staff, facilities, space...they don't want to admit that.
Don't get me wrong, I completely understand that those in power have to try to keep everybody calm at the moment, but I'd like the 'experts' to meet with more frontline staff.
Day 4:
This virus does not discriminate - age, race, lifestyle, it doesn’t matter. We are all at risk.
As shown last night, serious measures are now in place. But it’s so disappointing to see so many people ignoring the government’s advice. When I saw the pictures of crowded tubes in London today I wasn’t angry, I was bitterly disappointed. Clearly, people still don’t get this.
The restrictions are not to scare or frighten people, but to highlight the importance of staying at home and only mixing with people within the same household.
The situation on the frontline hasn’t changed much but we did manage to discharge a patient yesterday who had come to us with Covid-19. They no longer need support and can now manage the virus from home, which is really good to see.
In terms of Boris Johnson’s statement last night: I think we still have time now to get a handle on this. I think it took Boris a while to realise that maybe people had to panic in order for them to listen, and for him to get the message across.
We are getting a better structure in place - the people who are normally hiding away in the back offices are now out on the frontline, which is nice. We also have staff briefings every morning and evening and more space is being made available to deal with this - like the emergency theatre rooms.
Yes, everyone’s mental health is also going to be put at risk with the ‘lockdown’ announcement, but what you do with in self-isolation is key - exercise, find a new hobby, learn a new word daily!
We are in a time where social media is very prominent. Please use this to your advantage, daily meditation is being provided, home exercise with tins of beans! Don’t just don’t sit there scrolling through news feeds constantly.
As a nurse it is my duty and responsibility to keep up to date with the latest current affairs, however I’ve limited myself to only watching the daily 6pm news! It can get too much otherwise.
Please, please, please…You have to respect the requests to stay at home.
As shown last night, serious measures are now in place. But it’s so disappointing to see so many people ignoring the government’s advice. When I saw the pictures of crowded tubes in London today I wasn’t angry, I was bitterly disappointed. Clearly, people still don’t get this.
The restrictions are not to scare or frighten people, but to highlight the importance of staying at home and only mixing with people within the same household.
The situation on the frontline hasn’t changed much but we did manage to discharge a patient yesterday who had come to us with Covid-19. They no longer need support and can now manage the virus from home, which is really good to see.
In terms of Boris Johnson’s statement last night: I think we still have time now to get a handle on this. I think it took Boris a while to realise that maybe people had to panic in order for them to listen, and for him to get the message across.
We are getting a better structure in place - the people who are normally hiding away in the back offices are now out on the frontline, which is nice. We also have staff briefings every morning and evening and more space is being made available to deal with this - like the emergency theatre rooms.
Yes, everyone’s mental health is also going to be put at risk with the ‘lockdown’ announcement, but what you do with in self-isolation is key - exercise, find a new hobby, learn a new word daily!
We are in a time where social media is very prominent. Please use this to your advantage, daily meditation is being provided, home exercise with tins of beans! Don’t just don’t sit there scrolling through news feeds constantly.
As a nurse it is my duty and responsibility to keep up to date with the latest current affairs, however I’ve limited myself to only watching the daily 6pm news! It can get too much otherwise.
Please, please, please…You have to respect the requests to stay at home.
Please understand what I said at the start of this diary entry
This virus does not discriminate.
Day 3:
My hospital now has 150 confirmed cases of Covid-19. On Friday, we had 11.
It is impossible to say how many potential cases there are - Everybody at the hospital is now being screened so we will just have to wait and see.
We think that 25% of the UK population may already have Coronavirus. So for everyone still getting on a tube or train into work every morning - that carriage could be 25% Corona-positive.
While more supplies and funding have been made available to us, we are now having to make serious life and death decisions.
We have been told to prioritise those with a good chance of long-term survival, so they are the Covid-19 patients being intubated.
The death toll is likely to be higher than expected and the NHS is going to be stretched beyond capacity.
This is why people NEED to take the government’s advice seriously. If you stay at home and self-isolate for 14 days we can get through this. Just make sure you take this seriously.
Of course, we are still providing comfort care for people with serious underlying health issues, such as those going through chemotherapy, or anyone who was already likely to pass away as a result of their illness. But the strain on the NHS is immense.
It feels like every day we are becoming more used to this situation, but it doesn’t make it any easier to deal with.
It is impossible to say how many potential cases there are - Everybody at the hospital is now being screened so we will just have to wait and see.
We think that 25% of the UK population may already have Coronavirus. So for everyone still getting on a tube or train into work every morning - that carriage could be 25% Corona-positive.
While more supplies and funding have been made available to us, we are now having to make serious life and death decisions.
We have been told to prioritise those with a good chance of long-term survival, so they are the Covid-19 patients being intubated.
The death toll is likely to be higher than expected and the NHS is going to be stretched beyond capacity.
This is why people NEED to take the government’s advice seriously. If you stay at home and self-isolate for 14 days we can get through this. Just make sure you take this seriously.
Of course, we are still providing comfort care for people with serious underlying health issues, such as those going through chemotherapy, or anyone who was already likely to pass away as a result of their illness. But the strain on the NHS is immense.
It feels like every day we are becoming more used to this situation, but it doesn’t make it any easier to deal with.
Day 2:
The aim is to get the confirmed patients moved to specialist wards.
To see companies and professions outside of health care, providing support for NHS staff is a heart-warming.
New evidence and trends have been identified, patients are presenting with loss of smell and taste are testing positive for COVID-19.
A routine is being to develop at work, to some what mange this changing situation
To see companies and professions outside of health care, providing support for NHS staff is a heart-warming.
New evidence and trends have been identified, patients are presenting with loss of smell and taste are testing positive for COVID-19.
A routine is being to develop at work, to some what mange this changing situation
Day 1:
Today was the day it really hit home to me - this is a crisis. I had to go outside for about 15 minutes just to have a little cry.
We’ve had 11 confirmed cases of Coronavirus, 250 more are waiting for their results.
When a patient is tested a swab was taken from the back of the throat and nose. Indications can be seen on an x-ray by a radiologist but confirmation is needed from a positive swab for CoViD-19.
When a patient is tested a swab was taken from the back of the throat and nose. Indications can be seen on an x-ray by a radiologist but confirmation is needed from a positive swab for CoViD-19.
This is supposed to take 48 hours, but it is already taking 96 hours, regularly.
Staff are concerned that they aren’t being tested for Coronavirus and supplies are already running low.
Help researchers help you!
Take part in this novel research to make a change
- Share your opinion as your voice matters
- Help us understand everyone’s experience
- No bias, just science
- Help us improve future responses
AMO sends your votes securely via standard SMS, these are usually included free in UK airtime bundles. Ask your mobile supplier if you get inclusive SMS to standard UK mobiles.




